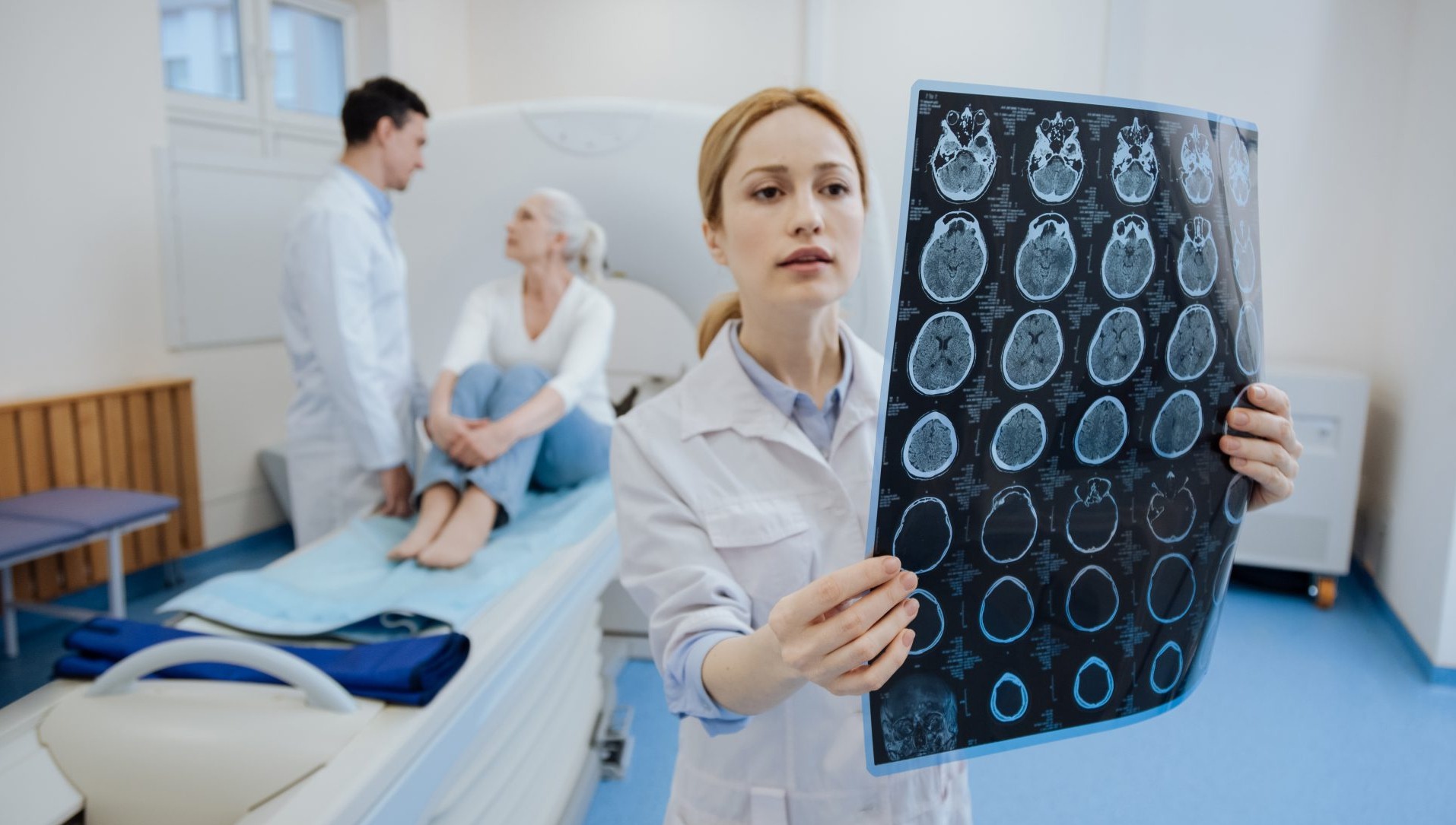
Technicalities of Neurology Clinical Trials
Neurology, the vast landscape of the brain and nervous system, holds both enigmatic complexities and hopeful possibilities. For individuals living with neurological conditions, clinical trials offer a glimmer of hope for improved treatments or even cures. But before embarking on this journey, understanding the intricate world of neurology clinical trials is crucial.
Microscopic Trial Design
Neurological trials differ from their counterparts in other specialties. The very nature of the brain, its intricate workings, and the delicate balance of its neurotransmitters pose unique challenges. Designing trials that accurately measure subtle changes in cognitive function, movement, or mood requires meticulous planning and specialized expertise.
Specialist neurologists and neuroscientists play a pivotal role in this intricate dance. They meticulously craft trial protocols, ensuring ethical considerations are paramount. Inclusion and exclusion criteria are carefully defined, balancing participant safety with ensuring representative samples. Blinding techniques, where neither participants nor researchers know treatment allocation, prevent bias and safeguard objectivity.
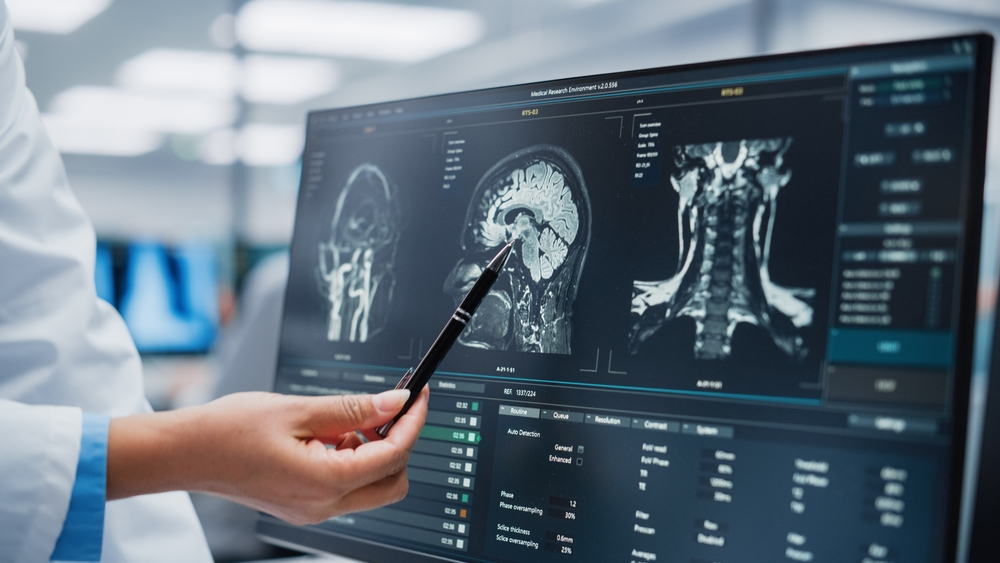
Technicalities Involved in Neurology Clinical Trials
Here are some additional technicalities to consider in neurology clinical trials:
1. Biomarkers and Neuroimaging: Measuring subtle changes in the brain can be tricky. Trials often rely on biomarkers, like blood tests or neuroimaging techniques like MRI or PET scans, to track disease progression and treatment response. However, choosing the right biomarker and standardizing its use across study sites can be challenging.
2. Endpoint Selection: Defining the primary and secondary endpoints, the measures of success for the trial, is crucial. In neurology, these could be changes in cognitive function, motor skills, mood, or survival rates. Choosing meaningful and sensitive endpoints that capture the real-world impact of treatments is complex.
3. Sample Size and Statistical Power: Determining the right number of participants for a trial is critical. Insufficient power could lead to inconclusive results, while unnecessarily large studies can be costly and time-consuming. Statistical models are used to calculate the required sample size, considering factors like disease prevalence and expected effect size.
4. Adaptive Designs and Bayesian Analysis: Traditional fixed-design trials have limited flexibility. Adaptive designs allow researchers to adjust the study based on interim data, making them more efficient and responsive. Bayesian analysis incorporates prior knowledge about the disease into the analysis, potentially providing more accurate results with smaller sample sizes.
5. Ethical Considerations in Vulnerable Populations: Neurological disorders often affect older adults or children, raising unique ethical concerns. Consent procedures must be adapted to their specific needs, and safeguarding their well-being throughout the trial is paramount.
6. Data Management and Sharing: The vast amount of data generated in neurology trials necessitates robust data management systems. Ensuring data quality, security, and privacy is crucial. In recent years, efforts to share data across studies are increasing, accelerating research progress.
These technicalities highlight the intricate dance between science, ethics, and technology in the world of neurology clinical trials. Understanding these complexities empowers patients and researchers alike to navigate this unique and impactful field.
Related Article: What Are Neuroimaging Techniques Advancements in Neuroimaging Techniques for Brain Research
Inside the Labyrinth: What are the Phases?
Just like embarking on an expedition, participating in a neurology clinical trial is a phased journey. Phase I trials, with a handful of participants, aim to assess safety and dosage. Phase II studies, involving slightly larger groups, delve deeper into efficacy and side effects. Finally, Phase III trials, with hundreds or even thousands of participants, provide robust evidence for regulatory approval.
But the path isn’t always linear. Some trials might skip phases or incorporate adaptive designs, dynamically adjusting to emerging data. Statistical analysis, the intricate language of interpreting results, becomes the compass guiding researchers through the maze of numerical labyrinths.
Twists, Challenges and Controversies
Despite the meticulous planning, unforeseen obstacles can arise. The elusive nature of neurological disorders makes measuring outcomes a complex ballet. Placebo effects, where participants experience improvement due to the study itself, add another layer of complexity. Ethical concerns around informed consent and vulnerable populations demand constant vigilance.
The recent Aducanumab saga, with its controversial approval for Alzheimer’s disease despite inconclusive data, highlights the need for robust regulatory oversight and transparency. Open communication between researchers, participants, and the public is paramount to navigate these ethical and scientific nuances.
Embracing the Future of Neurology Clinical Trials
Despite the challenges, neurology clinical trials remain beacons of hope in the quest for understanding and treating neurological disorders. From gene therapy for Parkinson’s disease to personalized medicine for epilepsy, the future holds immense promise.
Related Article: Neurologist vs Psychiatrist: What’s the Difference
Emerging technologies like artificial intelligence and advanced imaging techniques are poised to revolutionize trial design and data analysis. Patient-centric approaches, empowering participants to actively contribute to research, are gaining momentum.
For individuals considering participating in a neurology clinical trial, the journey might be daunting, but armed with knowledge and empowered by informed consent, they can become pioneers in shaping the future of neurological treatments. So, as you stand at the crossroads, ask yourself: will you step into the labyrinth, a willing participant in the grand experiment of unlocking the mysteries of the brain?
Sources:
- Nature Reviews Neurology: https://www.nature.com/subjects/neuroscience/nm
- PharPoint Research: https://pharpoint.com/services/clinical-trials/
- Mayo Clinic: https://www.mayoclinic.org/departments-centers/neurology/home/orc-20117057
- Vial: https://www.ncbi.nlm.nih.gov/books/NBK396103/